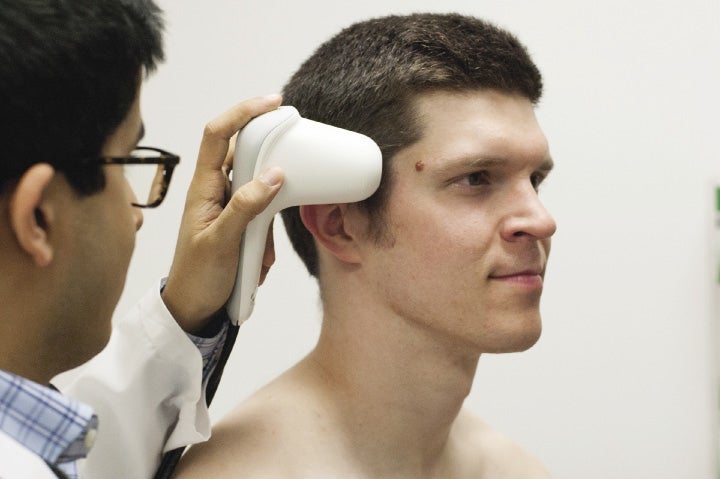
In years past, every skin rash or sore throat meant calling a doctor and trying to get in for the next available appointment. But now, digital screenings of medical conditions before an appointment – or in some cases, in place of one – are becoming more widespread.
The concept is called telemedicine, and it is basically the use of telecommunication or information technology to provide medical services remotely. Doctors can consult with, diagnose or treat patients using electronic media such as audio, video or advanced data monitoring services.
Though the first telemedicine technologies were released decades ago, its rollout has been somewhat limited in Massachusetts, according to the state Health Policy Commission. But it is becoming more widespread, as technology becomes more and more prevalent, health networks implement it and insurers adopt appropriate payment plans. Some health networks, including UMass Memorial Health Care, have implemented it successfully. The question of how to reimburse telemedical services is also being considered by the legislature.
Telemedicine isn’t a substitute for the longstanding doctor/patient relationship nurtured through years of physical visits, but it can supplement that, said Dr. Craig Lilly, professor of medicine, anesthesiology and surgery at UMass Medical School, and director of the eICU telemedicine program at UMass Memorial Medical Center. It can also be a time and cost saver, he said.
“For a lot of folks, the convenience of being able to access a camera or microphone allows prescribing physicians to make diagnosis and start a treatment plan with the same doctor we see in the office,” said Lilly.
Digitally monitoring patients
Lilly said the way he sees it, telemedicine breaks down into three forms. The first is when a patient gets remote care from a doctor he or she has an established relationship with. In that case, the provider knows a patient’s history and can give advice about a specific problem in the context of that prior relationship.
The second is in the case of an acute problem – like a rash, for example. An emergency room or primary care doctor might not know exactly what the rash is or where it came from. Instead of booking a specialist appointment for days or even weeks in the future, he or she could use telemedicine to bring in a remote expert, in this case a dermatologist, to provide an on-the-spot consultation.
“The difference is, right there, that day when you have it, you get the expertise … and you just move the whole calendar of getting the problem taken care of sooner. You get a definitive answer sooner,” Lilly said.
The third form would apply to a patient in an established healthcare system with an electronic health record. Telemedicine applies to the process of organizing the information, so an off-site physician or provider can help to make sure patients stay on track with their treatment plans established by a long-term care doctor.
The second and third forms depend on having a health information system that can electronically analyze health data, Lilly said.
“The electronic recording of basic medical information makes it easier for patients so they don’t have to repeat their story over and over again,” he said. The third form of telemedicine was the subject of research published in 2013 that included Lilly.
The 2013 study involved so-called eICUs, which pair voice, data and video monitoring technology with traditional bedside care. The advanced monitoring technology allows doctors and nurse practitioners to detect which patients are at-risk so they can monitor those patients and keep them from taking a turn for the worse. The study, which tracked 110,000 patients in 56 intensive care units in 32 hospitals nationwide, found patients who were cared for in the eICU were 26 percent more likely to make it out of the ICU and were discharged 20 percent faster than patients in traditional settings. The study was published in the journal CHEST in early 2014.
“The goal is for the patient’s bedside doctors to set a trajectory, and the role of the telemedicine team is to keep them on that trajectory,” Lilly said. “A second set of eyes, on almost any task, actually helps.”
Over the next three to five years, Lilly said he thinks telemedicine will expand mostly in primary care settings and emergency rooms.
“Electronics are increasingly present in our lives, and telemedicine is increasingly present in health care. It’s highly likely it will become more available in primary care offices, or when you’re in a hospital with serious illness,” he said.
Dr. James S. Gessner, president of the Massachusetts Medical Society, said his organization considers telemedicine a very important issue but that’s it’s not a replacement for the traditional, longstanding doctor/patient relationship.
The state Health Policy Commission announced in July the launch of a telemedicine pilot, geared towards expanding behavioral health telemedicine services, to remote areas. This was driven by an unmet need for mental health services statewide, HPC Executive Director David Seltz said.
The HPC last week awarded a $425,570 telemedicine pilot to Heywood Hospital in Gardner, and a pilot worth $496,184 to UMass Memorial Medical Center.
“We really focused our opportunity on the most vulnerable populations, and are excited to be able to leverage technology to address some of our biggest policy and public health challenges,” Seltz said.
Finding the right reimbursement
Although several healthcare networks and hospitals have implemented telemedicine technology, the method’s rollout in Massachusetts has been limited because of the way payers structured their coverage and regulatory provisions, according to a brief from the Health Policy Commission written last fall.
One of the ideas behind telemedicine is that it can be an effective tool to reduce costs in healthcare settings. There isn’t yet a statewide consensus on how to reimburse these services from an insurance standpoint.
Legislators discussed a bill proposing insurance reimbursements for telemedicine during the most recent legislative session. The bill suggests, instead of requires, that insurers reimburse telemedicine, and defines the term as the use of interactive audio, video or other electronic media for the purpose of diagnosis, consultation and treatment of a patient’s physical and mental health, and it excludes audio-only telephone, facsimile machine, online questionnaires, texting or text-only e-mail.
The bill does not require healthcare providers to document a barrier to an in-person visit in order to receive payment, and allows for deductibles, copayments or coinsurance requirements, as long as those telemedicine fees aren’t greater than fees for in-person services.
Any legislation produced at the state level regulating insurers would apply only to fully-insured plans, state-regulated plans which are usually adopted by small- to medium-sized employers and make up just 44 percent of private commercial enrollees in Massachusetts, said Eric Linzer, senior vice president of public affairs and operations at the Massachusetts Association of Health Plans. Citing data from the Center for Health Information and Analysis, Linzer said the remaining 56 percent of commercially insured people in Massachusetts have self-insured plans, which are federally regulated and normally adopted by larger companies.
The new bill, Linzer said, strikes a more appropriate balance than a previous version that required telemedicine be reimbursed at the same level as in-person visits. Still, the state shouldn’t dictate reimbursement levels, he said.
“We shouldn’t be dictating reimbursement rates in statute to being with – that was a significant concern we had with the bill because of potential impact is was going to have on the marketplace – but [the committee on] health care financing struck an appropriate balance,” Linzer said.
State Sen. Jim Welch (D-West Springfield) is the Senate chair for the Joint Committee on Health Care Financing. He said while the bill might only apply to some commercial plans, it’s a first step and could push the federal government in that direction.
“Oftentimes in Massachusetts when it comes to health care, we are on the forefront, the first ones to take bold steps forward,” Welch said.
Central Mass. pilot programs
Heywood Hospital and UMass Memorial Medical Center have received nearly $1 million in combined funds as part of a telemedicine pilot being conducted by the state. According to UMass Medical, the study using up to $496,184 in state funds will be used to connect patients with recovery coaches right at their bedside.
“We have already been able to develop psychiatric programs to help patients in the medical hospital while recovering from overdoses and from substance use and look forward to expanding this with an telemedicine capacity,” Dr. Alan Brown, vice chair of Adult Psychiatry Clinical Services at UMass Memorial, said in a statement.
The Edward M. Kennedy Community Health Center is one of two in Worcester implementing a pilot of 3derm, a teledermatology technology built by a Boston company of the same name. The co-founders want to create a system that could provide effective, 3-D photos of skin conditions to dermatologists, who determine if an office visit is needed.
“We first talked to doctor at Yale Medical, what he was saying, is they get pictures emailed all the time from patients, but it’s really hard to tell if that mole is suspect, or if it’s just the lighting the patient is under,” said Liz Asai, co-founder of 3derm.
So, 3derm came up with a 3-D imaging technology that cancels out all outside lighting, to provide an accurate picture so doctors can determine whether or not an appointment is necessary.
A study of 3derm technology by UMass Medical School found the technology to be just as effective at diagnosing skin conditions as in-person dermatologist visits. The pilot is taking place at nine health centers across Massachusetts. It will roll out at the Kennedy CHC by this fall, president and CEO Antonia McGuire said.
“[Telemedicine is] one of the next delivery waves of the future,” McGuire said.