Greater Worcester is projected to have among the worst shortfalls in the number of available hospital beds in the country, virtually no matter how hard the coronavirus pandemic hits.
The region doesn’t appear likely to come close to having enough space to meet the needs of those who would need any hospital bed, and in particular those needing to be in an intensive care unit, according to a Worcester Business Journal analysis on Thursday of Harvard Global Health Institute estimates conducted to help inform local responses to the pandemic.
The Worcester hospital referral region — which includes much of Worcester County — ranks in the worst 8% for Harvard’s projected shortage for total available hospital beds. It’s in the bottom 10% for intensive care unit beds.
The shortfalls — even if beds could be emptied of all other patients — could be massive: a need for more than 1,800 beds if just 20% of the population becomes infected with coronavirus and the peak of cases can’t be flattened beyond six months, compared to just 425 beds now typically available in the Worcester area.

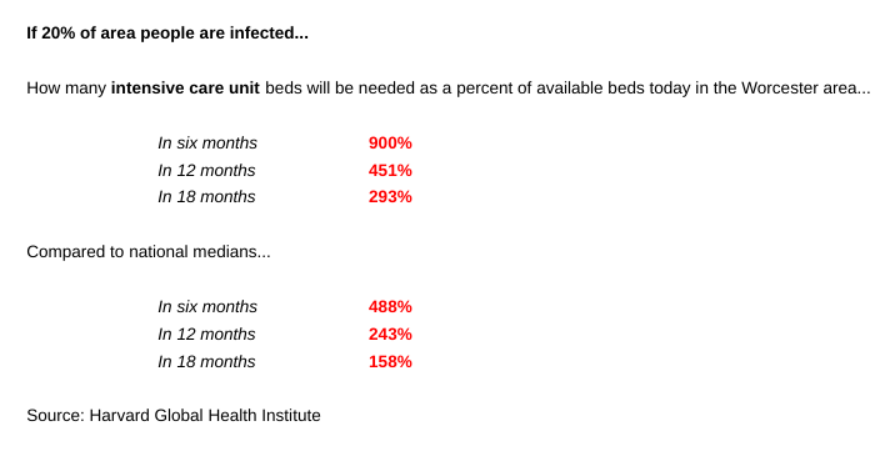
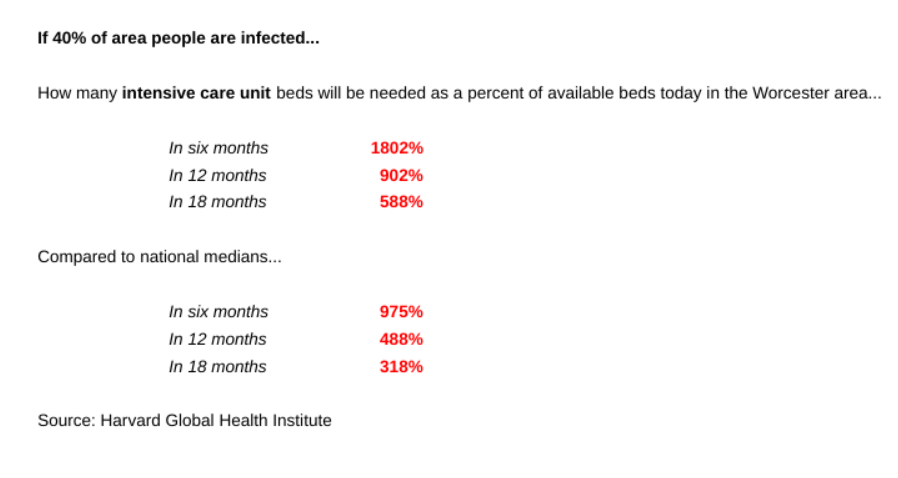
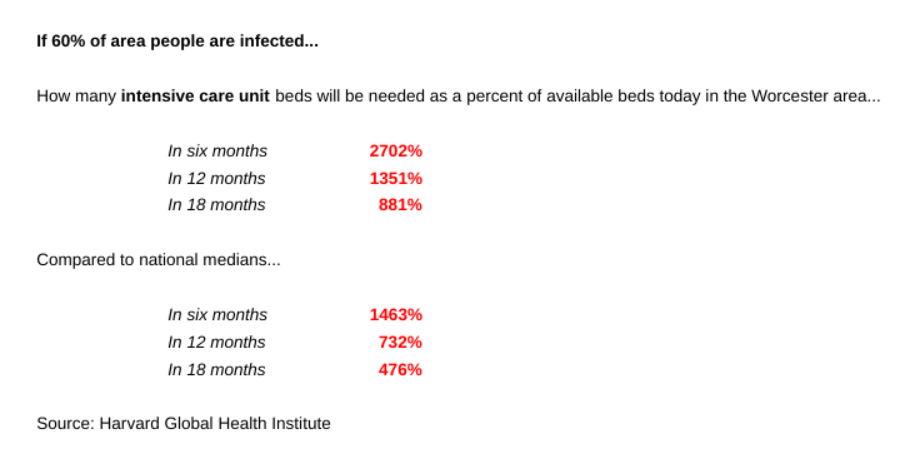
If 40% of the region is infected, 3,615 beds will be needed if the public can’t flatten the curve, the use the medical community’s term of lessening the peak of cases. At a 60% infection rate, the number of needed beds rises to 5,422.
Those rates are possible. Marc Lipsitch, a professor of epidemiology at Harvard’s T.H. Chan School of Public Health, has estimated that 40% to 70% of the world’s population could become infected.
Health officials have said flattening the curve, which minimizes how many people are infected at once, is critical to lessening the burden on hospitals. Doing so requires the widespread closure of businesses and schools and social distancing that has been put in place.
“Our goal is to give hospital leaders and policy makers a clear sense of when they will hit capacity, and strategic information on how to prepare for rising numbers of patients with COVID-19 needing care,” Dr. Ashish Jha, the director of the Harvard Global Health Institute, said in a statement.
Estimates were compiled through a range of factors, including how many total hospital beds and intensive care beds a region has, what percentage of beds are typically available, a region’s adult and 65-plus population, projected rates of infections and rates of those requiring hospitalization.

Through Thursday, the Massachusetts Department of Public Health reported 328 confirmed coronavirus cases, a jump of 30% in a single day. Gov. Charlie Baker has said he expects numbers to climb significantly as testing becomes more widespread.
Of the 328 cases, 43 — or 13% — have required hospitalization. Worcester County has so far had 14 reported cases.
Hospitals have already taken some action to add capacity by postponing most elective procedures in the coming weeks, and MetroWest Medical Center has indefinitely called off a plan to eliminate acute care services at its Leonard Morse Hospital in Natick.
[Related: Marlborough’s Quest ramping up coronavirus testing]
But the Harvard estimates show those steps may not come close to accommodating enough space — and that the space crunch could last for a year and a half.
In fact, even if only 20% of the Worcester area is infected, the region still wouldn’t have enough beds if the curve were to be flattened to 18 months instead of six, according to the analysis.
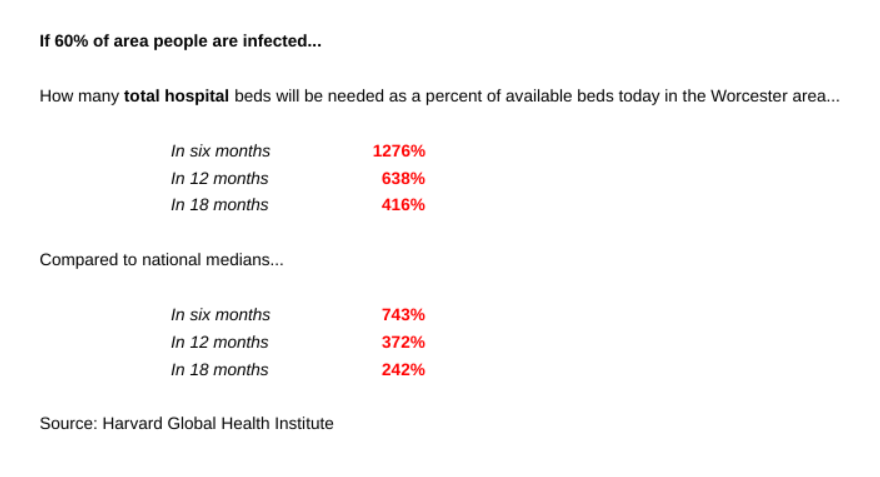

The worst shortfall, however, is due to take place in six months, giving hospitals in the Worcester area and nationally less time to figure out how to accommodate a projected rush of patients.
The Worcester region ranks 25th worst among 306 hospital referral regions nationally for total available hospital bed shortages, and 30th worst for intensive care bed shortages.
Most of Central Massachusetts is in Worcester’s hospital referral region, but much of MetroWest is in Boston’s and part of the Blackstone Valley is in Providence’s. Those areas, too, are slated to see major shortages.
Boston, for example, is 20th worst among referral regions for total hospital beds, and 114th for ICU beds. Providence is 38th worst for total beds and 48th worst for ICU beds.

Hospitals are already reporting shortages in some equipment, including in so-called N95 surgical masks at UMass Memorial Medical Center in Worcester, with hospital leaders advising practitioners to reuse masks for multiple patients if necessary. That step isn’t normally done but has been deemed acceptable for a limited time by the U.S. Centers for Disease Control and Prevention because of shortages.
Marlborough Hospital has asked the Corridor 9/495 Regional Chamber of Commerce for help obtaining face masks, face shielding and ventilators, according to the chamber. Hospitals have also reported blood shortages.
[Related: Shrewsbury CVS adding limited coronavirus screening]
The Massachusetts Nurses Association has lauded the delayed Leonard Morse Hospital closure and delaying unnecessary procedures but said there still appears to be a major shortage in capacity.
“The potential surge in volume of patients with possible exposure to or symptoms of COVID-19 illness still very much has the capacity to overwhelm our healthcare system,” the union said in a letter to Gov. Baker made public Thursday.
“The state should direct health care facilities to halt all planned bed, unit and facility closures. We should instead be looking at ways to increase capacity,” the group said.
The association has also called for all healthcare facilities, not only acute-care hospitals, to postpone or cancel all non-essential medical procedures, and to discharge patients as soon as practical.
CORRECTION: This story has been updated to more accurately explain how hospitals could be burdened with coronavirus patients. An earlier version described the number of beds needed at intervals of time of six, 12 or 18 months. According to the Harvard study, those are the number of beds needed if so-called flattening the curve were to be effective in extending the height of cases to those time periods, which would lessen the burden on hospitals.

